 For as long as she can remember, Allen School professor Su-In Lee wanted to be a scientist and professor when she grew up. Her father would sit her down at their home in Korea with a pencil and paper to teach her math — lessons that instilled not just a love of the subject matter but also of teaching. Today, and Lee is putting those lessons to good use in training the next generation of scientists and engineers while advancing explainable AI for biomedical applications. She is also adding up the accolades: After the International Society for Computational Biology recognized Lee with its 2024 ISCB Innovator Award and the American Institute for Medical and Biological Engineering inducted her into the AIMBE College of Fellows, yesterday the Ho-Am Foundation announced Lee as the 2024 Samsung Ho-Am Prize Laureate in Engineering. Read more →
For as long as she can remember, Allen School professor Su-In Lee wanted to be a scientist and professor when she grew up. Her father would sit her down at their home in Korea with a pencil and paper to teach her math — lessons that instilled not just a love of the subject matter but also of teaching. Today, and Lee is putting those lessons to good use in training the next generation of scientists and engineers while advancing explainable AI for biomedical applications. She is also adding up the accolades: After the International Society for Computational Biology recognized Lee with its 2024 ISCB Innovator Award and the American Institute for Medical and Biological Engineering inducted her into the AIMBE College of Fellows, yesterday the Ho-Am Foundation announced Lee as the 2024 Samsung Ho-Am Prize Laureate in Engineering. Read more →

Three is a magic number: Professor Su-In Lee earns trio of honors, including the “Korean Nobel Prize” in engineering, for advancing AI for biomedicine
 For as long as she can remember, Allen School professor Su-In Lee wanted to be a scientist and professor when she grew up. Her father would sit her down at their home in Korea with a pencil and paper to teach her math — lessons that instilled not just a love of the subject matter but also of teaching. Today, and Lee is putting those lessons to good use in training the next generation of scientists and engineers while advancing explainable AI for biomedical applications. She is also adding up the accolades: After the International Society for Computational Biology recognized Lee with its 2024 ISCB Innovator Award and the American Institute for Medical and Biological Engineering inducted her into the AIMBE College of Fellows, yesterday the Ho-Am Foundation announced Lee as the 2024 Samsung Ho-Am Prize Laureate in Engineering. Read more →
For as long as she can remember, Allen School professor Su-In Lee wanted to be a scientist and professor when she grew up. Her father would sit her down at their home in Korea with a pencil and paper to teach her math — lessons that instilled not just a love of the subject matter but also of teaching. Today, and Lee is putting those lessons to good use in training the next generation of scientists and engineers while advancing explainable AI for biomedical applications. She is also adding up the accolades: After the International Society for Computational Biology recognized Lee with its 2024 ISCB Innovator Award and the American Institute for Medical and Biological Engineering inducted her into the AIMBE College of Fellows, yesterday the Ho-Am Foundation announced Lee as the 2024 Samsung Ho-Am Prize Laureate in Engineering. Read more →
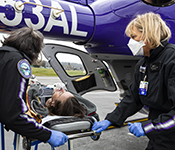
With CoAI, UW researchers demonstrate how predictive AI can benefit patient care — even on a budget
Allen School’s Gabriel Erion awarded prestigious F30 fellowship from National Institutes of Health
Gabriel Erion, an M.D.-Ph.D. student currently doing his Ph.D. research with Allen School professor Su-In Lee in the Artificial Intelligence for Medicine and Science (AIMS) Lab, has earned the prestigious Ruth L. Kirschstein National Research Service Award from the National Institutes of Health. The Kirschstein-NRSA, also known as the F30, was created to enhance research and clinical training of promising predoctoral students who are enrolled in a combined M.D.-Ph.D. training program and plan to pursue careers as… Read more →
